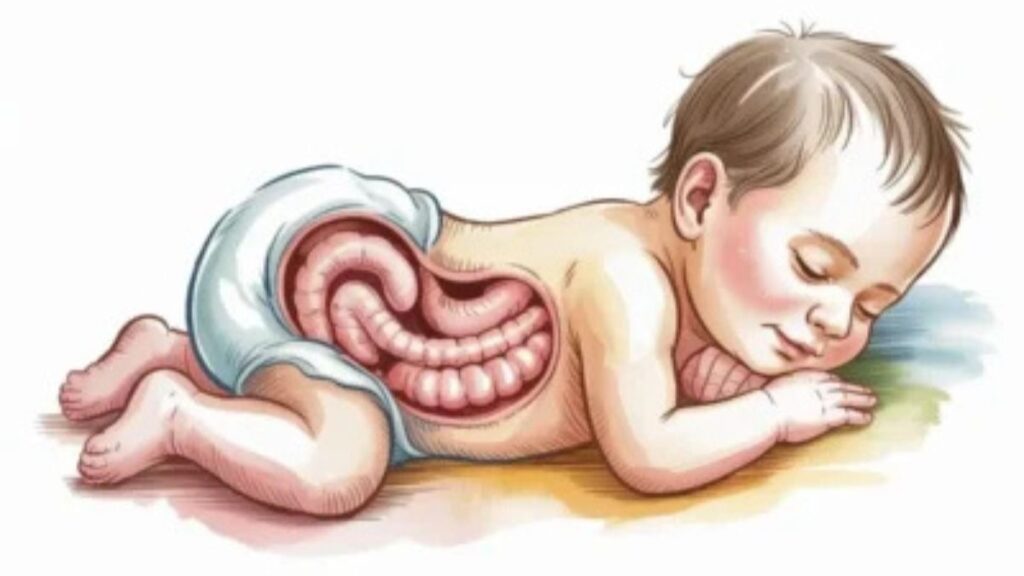
Introduction to Gastroshiza
Gastroshiza is a rare but serious congenital condition that affects newborns. It leaves parents with countless questions and concerns as they navigate the complexities of this medical issue. Understanding gastroshiza is essential for families facing this diagnosis, as knowledge can empower them during an uncertain time. In this article, we’ll delve into what gastroshiza is all about—its causes, symptoms, and treatment options—as well as how to cope with its challenges. Whether you’re a new parent or just seeking information, we’re here to guide you through the essentials of gastroshiza in an approachable way.
What Causes Gastroshiza?
Gastroshiza occurs when a baby’s abdominal wall fails to close properly during development. This defect leads to the intestines protruding outside of the body. The exact cause remains unclear, but several factors may contribute.
Genetic predispositions play a role in some cases. Family history can heighten the risk for future pregnancies. Environmental influences are also under investigation, including exposure to certain medications or substances during pregnancy.
Nutritional deficiencies in mothers could potentially impact fetal development as well. Folic acid deficiency has been noted in research surrounding various congenital disabilities.
Furthermore, maternal age is a factor that cannot be overlooked. Women over 35 years old have a slightly increased likelihood of having children with gastroshiza and other similar conditions.
Understanding these causes helps researchers develop better preventive measures and treatments for this complex condition.
Signs and Symptoms of Gastroshiza
Gastroshiza presents several distinct signs and symptoms that are crucial for early identification. In newborns, the most noticeable feature is the protrusion of abdominal organs outside the body through a defect in the abdominal wall.
This condition often leads to visible intestines or other organs lying exposed. The severity can vary; some infants may have only a small section of the intestine affected, while others might present with more extensive exposure.
Affected babies may also experience feeding difficulties shortly after birth. This can result from both physical challenges and potential complications related to organ function.
Additionally, parents may observe discomfort or distress in their child due to the unusual positioning of internal structures. Rapid medical attention is essential for managing these symptoms effectively and ensuring adequate care for affected infants.
The Diagnosis Process for Gastroshiza
Diagnosing gastroshiza involves a series of careful evaluations. It often begins during pregnancy when an ultrasound reveals abdominal wall defects in the developing fetus.
Healthcare providers may conduct additional imaging studies, such as high-resolution ultrasounds, to assess the extent of the condition. These scans help visualize any organs that might be outside the abdominal cavity.
After birth, physical examination plays a crucial role. Doctors will examine the newborn for visible signs and confirm whether other abnormalities are present.
Genetic counseling can also be beneficial. Understanding family history may provide insights into potential genetic factors associated with gastroshiza.
In some cases, further tests might be necessary to rule out other conditions or complications related to this defect. Through these steps, healthcare professionals ensure an accurate diagnosis tailored to each individual situation.
Treatment Options for Gastroshiza
Treatment for gastroshiza typically begins with surgical intervention shortly after birth. Surgeons aim to return the intestines into the abdominal cavity and close any openings in the abdominal wall.
In some cases, a staged approach may be necessary. This involves initially covering the exposed organs with a protective sac before gradually repositioning them later as the child grows stronger.
Nutritional support is also crucial during recovery. Many infants require specialized feeding methods, such as intravenous nutrition or tube feeding, until they can eat normally.
Long-term management may involve monitoring for potential complications like bowel obstruction or infections. Pediatric specialists will guide families through these challenges while providing ongoing care tailored to each child’s needs.
Emotional and psychological support plays an important role too; connecting with other families facing similar situations can foster resilience and understanding on this journey.
Coping with Gastroshiza: Lifestyle Changes and Support Resources
Living with gastroshiza can be challenging, but there are ways to adapt and thrive. Making certain lifestyle changes can help manage symptoms and improve overall well-being.
Focusing on a balanced diet is crucial. Nutrient-rich foods can support healing while minimizing gastrointestinal distress. Consulting with a nutritionist may provide personalized guidance tailored to individual needs.
Emotional health plays an essential role in coping. Joining support groups allows for the sharing of experiences and advice with others who understand the journey. Online forums and local meetups create connections that foster resilience.
Routine medical check-ups are vital for monitoring progress. Staying informed about potential complications helps parents feel more empowered in managing their child’s care.
Encouraging open communication within families creates a supportive environment where feelings can be expressed freely without judgment or fear. This strengthens bonds during difficult times, making the experience less isolating.
Future Developments in the Treatment of Gastroshiza
Research into gastroshiza is evolving rapidly, offering hope for improved patient outcomes. Scientists are exploring innovative surgical techniques that may reduce recovery time and enhance the success rate of repairs.
Advancements in prenatal diagnostics also play a pivotal role. Enhanced imaging technologies can identify gastroshiza earlier in pregnancy, allowing families to prepare better and healthcare teams to develop tailored treatment plans.
Additionally, regenerative medicine is gaining traction. Stem cell therapies could potentially aid in tissue repair post-surgery, minimizing complications associated with traditional methods.
Collaboration between researchers and medical professionals is crucial. This collective effort promises to refine existing treatments while paving the way for novel approaches that could change how gastroshiza is managed.
As knowledge expands within this field, patients might experience less invasive options and improved overall care strategies moving forward.
Conclusion
Gastroshiza is a complex condition that requires understanding and awareness. It affects many infants, presenting unique challenges for families. By recognizing the signs and symptoms early on, parents can ensure timely medical attention.
Diagnosis often involves imaging tests like ultrasounds, which help confirm the presence of this defect. Treatment options vary but may include surgical intervention to reposition the intestines into the abdominal cavity.
Coping with gastroshiza goes beyond just medical treatment. Families benefit from lifestyle changes and support networks that provide emotional assistance during difficult times.
As researchers continue to explore new therapies and interventions, there is hope for improved outcomes in those affected by gastroshiza. Awareness and education remain crucial in navigating this condition effectively, ensuring both patients and families receive the care they need as they move forward on their journey toward health.